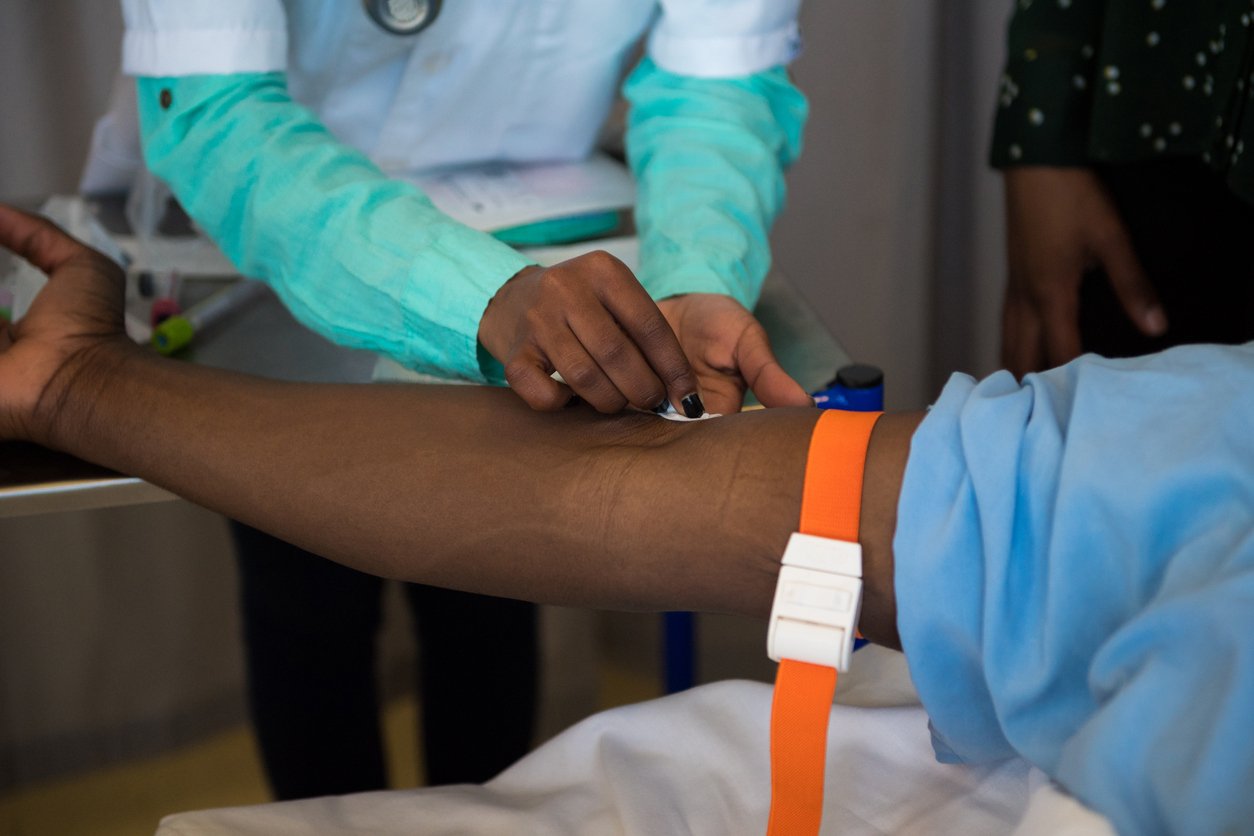
Providing information is a way to influence health behaviour, but traditional medical beliefs may hamper learning about hygiene and other ways to prevent disease. This column reports on the impact of an initiative to inform rural women in Pakistan about microbes. Showing participants germs under a microscope enhances the impact of instruction on hygiene – but not for women with strong beliefs in Unani, the predominant form of traditional medicine in Pakistan.
Providing information is an important way to influence health behaviour. Messages run the gamut from campaigns to stop smoking to HIV testing programmes. The information might be delivered by healthcare providers, billboards or television programmes.
To work as intended, health messages must be convincing. But while healthcare professionals may presume that patients take their advice to heart, official health messages can conflict with messages from other sources.
Hygiene promotion in Pakistan offers a telling example. As in many other developing countries, diarrhoea is an urgent threat to infants and young children. Hygiene promotion programmes typically combine subsidies for soap, latrines or other goods, with educational messages about hand washing, water purification and safe food handling.
Hygiene messages typically invoke the germ theory of disease, which states that invisible microbes cause infectious diseases like diarrhoea. The germ theory is a relatively recent discovery that only gained traction in the 1880s through the work of Louis Pasteur and others. Throughout the world, it competes with non-pathogenic disease models from alternative, traditional and folk medicine. In the United States, for example, 40% of adults use at least one form of alternative medicine. The World Health Organization reports that traditional medicine constitutes around half of healthcare use in China and up to 80% of healthcare use in sub-Saharan Africa.
In Pakistan, many people practice Unani medicine, which dates back to the eleventh century and is based on the teachings of Hippocrates and Galen. In this system, diseases arise through imbalances among the four humours of blood, mucus, yellow bile and black bile, as well as the four qualities of heat, cold, moisture and dryness.
Similarly, Ayurveda and Traditional Chinese Medicine invoke the concept of balance. For someone with limited exposure to science, non-pathogenic disease models may seem plausible while the notion of infection by invisible microbes may seem fanciful.
In the Unani system, diarrhoea is a ‘hot’ illness, although hot and cold designations do not correspond to physical temperature. A person can prevent and treat diarrhoea by reducing exposure to objects, foods and activities that are hot while increasing exposure to those that are cold. Since working outdoors makes a mother’s breast milk hot, Unani doctors advise women with diarrhoea to withhold milk from their infants, in contrast to the Western approach of oral rehydration therapy. A women’s sympathy for this or other medical models may influence how she responds to health information such as the recommendation to prevent diarrhoea by washing hands.
Microbe Literacy (ML) is a novel hygiene education programme that attempts to surmount the lack of familiarity with microbes. Like other hygiene education campaigns, the programme provides instructions on hand washing, safe food handling and other aspects of communicable disease prevention.
Prior to delivering these messages, facilitators use microscopes to show participants the microbes in everyday substances such as standing water and buffalo dung. This demonstration, which is eye-opening for many people, may make subsequent hygiene messages more credible.
In a new study, Asjad Naqvi, Wolf-Peter Schmidt and I evaluate the impact of this programme on hygiene and child health. In 2013-14, we collaborated with the Microbe Literacy Initiative to offer ML to women in existing adult literacy classes in southern Punjab Province, Pakistan. We selected 210 classes (containing 4,032 participants) and randomised the classes into arms that received the full ML programme, only hygiene instruction (without the microscope demonstration) and neither intervention.
We followed up after four months and 16 months to measure the impacts on hygiene, sanitation, child health and anthropometrics. In both follow-ups, ML participants exhibited significantly better hygiene than participants in either of the other groups. Effects on sanitation were insignificant after four months but grew and became significant after 16 months. Effects on child health and anthropometrics were positive but not significant overall.
The additional impact for ML participants shows that the microscope demonstration magnified the impact of the health information. To explore this finding further, we examined differences in the strength of participants’ Unani beliefs. We elicited beliefs in several Unani ideas related to diarrhoea and divided the sample into groups with weak and strong traditional medical beliefs. The distinction was striking. Respondents with weak beliefs exhibited large and significant impacts on hygiene and child health, while those with strong beliefs barely responded.
This heterogeneous response suggests that traditional medical beliefs may hamper learning about hygiene and other forms of disease prevention. This trade-off could arise in several other contexts. For example, the message to use condoms to prevent HIV is less persuasive if witchcraft causes AIDS; the message to avoid air pollution is less compelling if herbs can purify and restore your body.
This topic is therefore pertinent to global health as billions of people throughout the world follow traditional medicine. Yet very little research considers the substitution between traditional and Western medical beliefs and expenditures. The extent of substitution surely varies by illness, traditional medical system and other contextual factors. Proponents of Western medicine should recognise that people may not accept messages based on the germ theory at face value, and should take proactive steps to overcome this scepticism.